Scientists have taken note of recent reports which say air conditioners may have served as a conduit in intensifying the spread of COVID-19 in Wuhan, the first epicentre of the disease.
It has been reported that split air conditioners – commonly used in homes – may have trapped the virus inside rooms.
The findings have prompted a rethink of how conventional air conditioning systems should be designed not only to produce cool air but also to provide optimum safety against diseases. A new air conditioner which has redesigned mechanics would be ideally suited for tropical countries such as Thailand, observers say.
The treatment of Covid-19 patients has given us a glimpse of how the air conditioning hardware of tomorrow can save lives.
People are growing increasingly familiar with the terms “negative pressure” and “positive pressure” used to describe special chambers in hospitals specifically for COVID-19 patients.
Special chambers are rooms designed to serve two purposes. In a positive pressure environment, the potentially virus-tainted air outside is kept at bay; however, the chamber can also be converted into a negative pressure environment to prevent the air inside the room of infected patients from escaping outside.
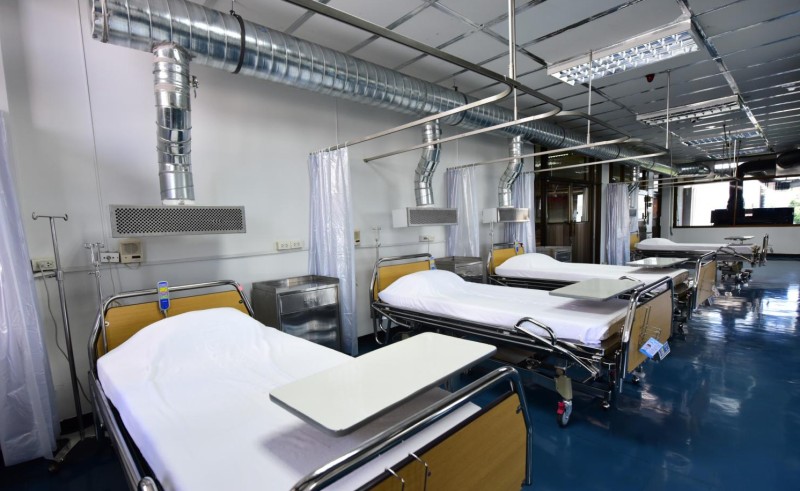
On April 20, the Centre for COVID-19 Situation Administration (CCSA) announced the opening of the country’s first negative pressure operated cohort ward at Phramongkutklao Hospital in Bangkok.
CCSA spokesman Taweesilp Visanuyothin said the ward, which occupies two floors of the building, required modifications of the interior and was equipped with a pressure system for taking care of COVID-19 patients.
The modification was undertaken jointly by Saijo Denki, a manufacturer of air conditioners, and the King Mongkut’s University of Technology Thonburi. The conversion project took three weeks to complete and the result was a ward – large enough to fit 40 beds – that is entirely pressure-adjustable.
“The ward provides room for coronavirus patients with mild symptoms to be accommodated together in large rooms to save resources,” Dr Taweesilp said.
“The air inside is also filtered to create a constant supply of clean air within the ward,” Dr Taweesilp added.
Preeyanant Jarujinda, deputy director of the Phramongkutklao Hospital, told the Bangkok Post the so-called “true negative pressure” feature inside the ward generates cool air and controls humidity with a high level of precision that conforms to the standards set by the World Health Organization and the Centers for Disease Control and Prevention (CDC) in the US.
Tainted air in the ward is piped into the High-Efficiency Particulate Air (HEPA) filter and is thoroughly cleaned.
Dr Preeyanant said plans are afoot to develop more dual-feature operating theatres which can deploy either a positive or negative pressure environment.
She said that ideally, a cohort ward should at least operate with negative pressure. However, the rapid spread of COVID-19 has not given hospitals enough time to prepare their facilities for this type of treatment.
Instead, some have made do with using a plastic-covered contraption which is placed over a patient’s bed to create an individual negative-pressure unit.
“It’s cheaper to build, however, it can be rather uncomfortable for the patient and awkward for doctors to deliver treatment inside the cocoon,” she said.
As the outbreak was intensifying, hospitals were racing against time to find a place that could be quickly transformed into a cohort ward as infections surged by the day.
Dr Preeyanant said the cohort ward was made where previously there used to be a trauma unit for accident victims situated on the fourth and fifth floors of the building. The ward, the biggest of its kind in the country, is isolated from the rest of the hospital to maintain optimum health safety.
“The infection tally has stabilised in recent weeks, which is quite reassuring,” Dr Preeyanant said.
Apart from the cohort ward, the hospital also has five rooms in its intensive care unit which run on negative pressure.
Meanwhile, Somsak Chittipalungsri, managing director of Saijo Denki International Co, said the company conceived the idea of developing the system to fight communicable diseases when the Severe Acute Respiratory Syndrome broke out in 2003.
The company has since patented the anti-disease system and several components in its air conditioners.
In an interview with the Bangkok Post, Mr Somsak said the cohort ward conversion was designed around the key consideration of where the air will enter and exit the ward. This has to do with the physical positions of the patients’ beds and where the doctors enter the room.
Installing the air filtering system at the cohort ward cost B26 million. However, the company covered the cost in a bid to help curb the spread of infections.
Mr Somsak said the treatment chambers could set the tone for the “new normal” associated with the post-coronavirus production of new models of air conditioners.
“Let us not forget that genuinely clean air cannot be produced simply by filtering or disinfecting it.
The trick is to draw in fresh air from outside, let it circulate in the room and filter it before releasing the air back into the open environment which is something the common split-type air conditioners cannot do,” Mr Somsak said.
The typical air conditioners in people’s homes only pull in outside air, and along with it, a certain degree of heat and humidity which can breed fungus and bacteria.
To ensure only clean air enters a room, it must be replaced at least 14 times by outside air each day. However, that means the filter and compressor in the air conditioning system must work constantly, which is certain to cause electricity bills to skyrocket, he said.
However, if the air conditioning system at the COVID-19 cohort ward can be emulated in the common air conditioners – which are then mass-produced – their retail price could be made affordable.
This will ensure people will be able to breathe cleaner air in their homes.